|
Age, sex, race, serum sodium, creatinine, INR, bilirubin, albumin, and height were considered for inclusion in the model. As such, ascites and encephalopathy were excluded from the model development. In the selection of the variables, the same principle was used as in the original MELD score that the variables must be measurable in an objective fashion and generalizable. A wide array of variables was extracted as potential predictors of waitlist survival, including demographic information, components of MELD and CTP scores, and additional laboratory parameters. The cohort was then randomly divided in a 70:30 ratio into model development and validation data sets. These inclusion and exclusion criteria were consistent with prior iterations of the MELD score. Patients listed for (1) multi-organ transplant, other than simultaneous liver-kidney transplant, those with (2) history of previous liver transplant, and those with (3) exception points at the time of registration, were excluded. The primary inclusion criteria for the analysis were (1) adults aged 18 years or older (2) registered for primary liver transplant with (3) end-stage liver disease. Out of the data set, we created a cohort of liver transplant candidates newly waitlisted between and. For the purpose of the analysis, the OPTN data, consisting of liver transplant candidates waitlisted in the United States, represent the population to which the results are directly applicable. The main portion of this analysis was performed on the OPTN Standard Transplant Analysis and Research (STAR) files with data curated as of. Under the current urgency-based liver allocation policy in the United States, the role of the MELD score is to inform the organ allocation system of the biological predictors of mortality, independent of the transplant policy and practices that could also affect waitlist outcome, such as donor-recipient size matching, geography, or healthcare access to transplant. 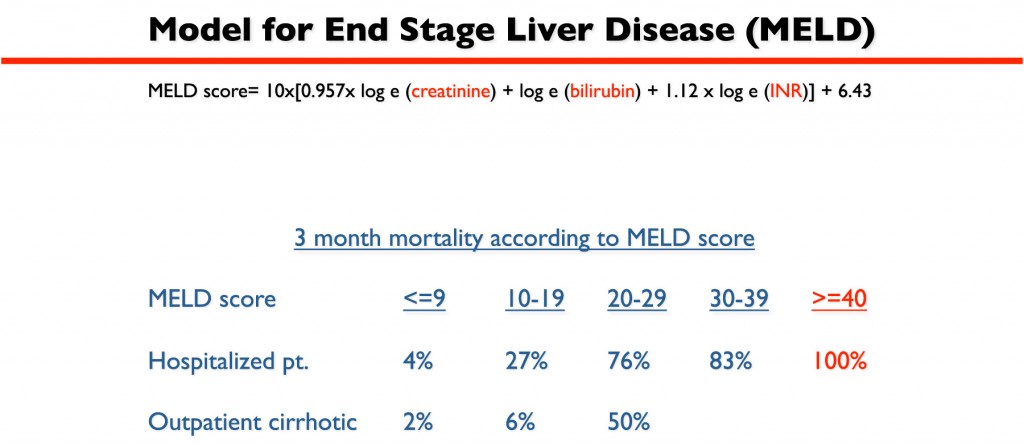
Some of the principles that guided our work included (1) consideration of biomedical insight in addition to statistical significance in determining model parameters, and (2) incorporation of objective, generalizable and easily verifiable variables. In this work, we set out to investigate whether the fit of the MELD score could be further optimized by considering alternate coefficients or by including additional variables in predicting short term mortality in the modern era. 6 Similar to ascites and encephalopathy, however, these variables are not as objectively verifiable as laboratory data, making them difficult to be included for the purpose of allocation. 5 A relevant, recent example may be sarcopenia and frailty, which have been consistently associated with poor prognosis in patients with many chronic illnesses including end-stage liver disease. Thus, while the Child-Turcotte-Pugh (CTP) score has proven to be a highly useful clinical tool to assess severity of hepatic decompensation, the advantage of MELD is that the data elements are verifiable and auditable for policy implementation. An important historical perspective is that a large part of the acceptance of MELD was the lack of variables that could be subjectively interpreted. A common approach is to incorporate additional variables. 4Įven before these observations were reported, many attempts have been made to improve MELD. In addition, there has been a growing concern that women are disadvantaged in the current system for a number of reasons, including serum creatinine overestimating renal function in women and thus underestimating their risk of mortality. 3 There may be a number of potential reasons for the concern, ranging from changes in liver disease epidemiology and development of therapies that alter disease prognosis to changes in the distribution of MELD scores and increasing age and comorbidity in patients awaiting transplant. More recently, questions have been raised whether the accuracy of prediction of mortality by MELD may have decreased.  
MELDNa has been utilized to determine priorities for allocation of livers for transplant in the US since 2016. 1 The current version of the MELD score, commonly referred to as MELDNa, incorporates serum concentrations of total bilirubin, creatinine and sodium, and the international normalized ratio (INR) of prothrombin time. Since its original description, the Model for End-Stage Liver Disease (MELD) has proven to be a reliable predictor of short-term survival in patients with end-stage liver disease.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
